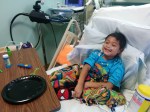
As many of you know, Patrick had an appointment for a check-up at Seattle Children’s this week. He was scheduled in clinic for about two hours Tuesday afternoon. We decided to try to make a family vacation out of this trip (since we haven’t had a vacation since adopting Patrick.) I think we need to stop saying the word vacation in our household. It seems that Patrick thinks that vacations are taken in the hospital – this trip did not go as planned.
We flew to Seattle on Sunday. We rented a mini van and drove to visit our good friends, the Laylands who live half an hour north of the city. We had a good dinner and visit with them and then spent the night at their house.
As soon as the plane touched down in Seattle, my nose started to run. At first I was sure it was allergies, but by the next morning there was no question that it was a cold. But, we were determined to have a vacation, so after a quick stop at K-Mart for some cold medicine and other things, we set off for the city.
After picking up some much touted Mighty-O donuts and checking into our hotel, we headed to the Seattle Aquarium. We were in the first exhibit, a sort of aquatic petting zoo, letting Patrick play in the water and touch sea creatures when I looked down and noticed blood on his PICC line. Closer examination revealed that there was something wrong … there was definitely a leak.
So I made a quick call to our transplant coordinator and we headed back to the ER, leaving a very patient Lindy and her daughter stranded in downtown Seattle to avoid exposing them to hospital ER germs.
We were checked in quickly in the ER and sent to an isolation room at the back because of Patrick’s and my cold symptoms. Soon the IV team came to look and confirmed that Patrick did, indeed, have a cracked PICC line. And it could not be repaired.
As a result, Patrick needed to have a peripheral IV put in until he could get another central (goes to the heart) line. And he needed to be admitted to the hospital because you can’t get as good of nutrition through just a hand or foot.
Wednesday afternoon, there was finally room in the schedule to take Patrick to “Interventional Radiology” where they could place a new PICC line with X-ray imaging to guide them. They took Patrick down at about 3 p.m. At 5:30, a doctor came to the room to talk to us.
He explained that they had tried to pass the wire through Patrick’s vein to put in the PICC line and had run into resistence. So, they injected contrast into his veins and saw that there had been a clot. In response to the clot, Patrick’s body created a branch of smaller vessels to route the blood where it needed to go. This meets the body’s need, but doesn’t leave enough room to put a catheter into the vein to the heart. Because of this, Patrick can no longer have PICC lines in his arms.
They put a little bit more stable of a line in his arm then that wouldn’t go bad as quickly as an IV in his hand or foot and then gave us two options: stay here and have a broviac line put in, or fly to Salt Lake, be admitted there, and have a broviac put in.
We decided that it was best to just stay and have it done here in Seattle. The surgeons here had gone into the PICC placement procedure and had seen the problem first hand. Having Seattle Children’s put in the line also meant that he’d have it done sooner, since he could be put on the next day’s list.
Beyond that, in order to place the line, they needed to do an ultrasound study to see what Patrick’s remaining central blood vessels looked like. Since not having many available blood vessels moves you up the transplant list, we thought it was wise to have the transplant hospital have a record of what options remained.
So – yesterday Patrick had a new broviac line put in. He went to surgery about 3 p.m. and they were able to put the new line right where they wanted it. When I talked to the surgeon at 5 he sounded pretty good about how the procedure had gone.
There had, however, been one slight problem. Patrick’s stomach still doesn’t easily drain all the way. Even though he hadn’t eaten anything, and his stomach had been suctioned, it still wasn’t empty. As a result, he aspirated during the procedure. The surgeon said that they’d been able to clean out his lungs, though, and didn’t seem overly concerned. With any aspiration, there is a risk of pneumonia. He asked to keep Patrick 24 hours for observation, and then said he’d be able to go home.
I went to Patrick’s room to wait for him. When he finally made it upstairs, he was very upset. He’d curled himself into a little ball and was crying miserably. The nurse immediately set to work getting pain medications for him. And we decided to put him on monitors.
Things just seemed to get worse. The monitors showed that the oxygen levels in his blood were dropping, so we put an oxygen mask near his mouth to help keep them up. His heart rate was rising. He was breathing very heavily.
The nurse called in other nurses to help her and started taking vitals… And discovered Patrick was running a fever. They called down his doctors. While I explained the scarier things in Patrick’s medical history, his nurse wandered around the room making space to work if things got worse.
They ordered blood cultures to look for infection, gave Patrick some Tylenol, and got an X-ray of his chest.
Finally, they called the “Rapid Response Team”, which is a team from the PICU who come to the bedside. They watched him, took some tests bedside, and promised to come back to check on him within the hour.
Once all of the tests were done, I picked Patrick up again and he finally started to calm down. They started antibiotics while I rocked him to sleep. His heart rate was still high, and the antibiotics were making his blood pressure low, but he seemed to be starting to feel better.
As things started to settle down, I asked the nurse to help me reach elders from my church. One of the doctors in the room had mentioned earlier in the week that he had gone to school at BYU and we’d talked about how we’d been there the same year both studying Spanish. He spoke up and said “I can take care of that for you.” It was subtle, but we both understood that he was telling me that he was an elder and could help me with what he knew I was going to ask for.
In the Church of Jesus Christ of Latter Day Saints we believe in the gift of healing by the laying on of hands by those who have authority from God. Brian is an elder in our church and had given Patrick one of these special blessings before he left. And this kind doctor subtly waited around until the nurses had left the room and then layed his hands on Patrick’s head and gave him another blessing, confirming the promises of health and comfort and strength.
Patrick slowly began turning around. His fever dropped and he started to sleep comfortably. A respiratory therapist came and tried to get Patrick to cough by pounding on his chest and back. Finally, she suctioned deep down into his chest and helped to get a lot of what was in his lungs out.
By midnight, Patrick was sound asleep. I stayed up to help the nurse get a few more things settled and went to bed. We slept till 7 a.m., when the doctors came in to check on him.
This morning, Patrick woke up with a smile. He was a bit weak and groggy at first, but has just gotten better and better all day long. Just an hour ago, he was climbing all over me on the couch in the room playing with toys and jumping. You would never know anything had been wrong.
The doctors are pleased enough with his improvement that they gave me the go ahead to book a flight back home for tomorrow. We’ll leave the hospital a little after noon to catch a 3:45 p.m. flight. We should be home by 6 p.m.
I almost hate to write this because any time I’ve said that we were doing something this week, things have changed. But this time it feels like we really are going home. And I’ll be happy to be there.
I do have to share one example of the goodness of people in this world. While Patrick was in surgery, I put some of our clothes in the laundry room here. I got it as far as the dryer, but then when Patrick came back in such bad shape from surgery, didn’t make it back to it. I expected, when I headed back at midnight, to find my clothes piled in a basket somewhere. Instead, someone had taken the time to neatly fold them for me. This touched me because any parent using the laundry room here is doing it because their child is sick enough that they’re expecting to stay here for some time. The person who folded my clothes was certainly going through their own difficult time and would have been totally justified in being upset and offended at someone leaving clothes in a dryer. Instead, they took the time to make my day a little better.
This is just one example of the kindnesses that make raising a child with health problem so very rewarding.
 Patrick finally got some good sleep last night. In fact, he was well on his way to sleeping all day. At 10 a.m., he had succeeded in going back to sleep again no matter the interruption. Therefore, I was in my PJ’s with hair uncombed when the team came for rounds.
Patrick finally got some good sleep last night. In fact, he was well on his way to sleeping all day. At 10 a.m., he had succeeded in going back to sleep again no matter the interruption. Therefore, I was in my PJ’s with hair uncombed when the team came for rounds.