Patrick discovered a couple of weeks ago that his activity center is a jumper. Since then, he has jumped at every possible opportunity.
Patrick discovered a couple of weeks ago that his activity center is a jumper. Since then, he has jumped at every possible opportunity.
We always stall as long as possible between Patrick’s haircuts, just cuz we love his little mophead. However, Patrick had hair in his eyes in front and his hair was past his collar in back… all except the very back of his head where he’s rubbed all the hair off while scooting around.
This is the best before picture he’d allow. His eyes are closed because he didn’t like the mist from the water bottle.

Most of the haircut was patient waiting, with a few wiggles.
Of course, he did start to get sleepy by the end.
But in the end, still turned out quite handsome.
Thanks to Wes of The Hair Place for a great haircut. And for keeping Daddy looking nice, too.
I’m writing from Primary Children’s hospital again. Tuesday afternoon, Patrick started to act as though he had an upset stomach. I got him settled and he took a nap, but before long woke up upset again. So, as I always do, I took his temperature and lo and behold, he had a fever.
I made a call to the GI on call, Dr. Pohl, and he made arrangements for us to check in to the hospital directly, without going through the E.R.
It was strange to come in without the E.R. routine, but kind of nice, too. The infant unit was full, so they put us in a room in the Children’s Medical Unit just down the hall. As usual, the first few hours were chaos as I gave history, got meds and supplies ordered, and generally got acquainted with the medical staff.
Typical protocol is to draw blood cultures to look for and identify the infection he has. So they call IV team and they draw blood from a vein while the nurse is responsible for drawing blood out of Patrick’s PICC line. They also draw blood to check levels of other important things like blood sugar and electrolytes through his PICC.
Well, Patrick’s PICC line has been tricky and occassionally with clot and not draw back. In this case, neither lumen would draw back. So about 11 p.m. they started soaking it in something to break up clots… but it still wasn’t working.
Finally at midnight things were pretty quiet, even though they didn’t have labs, and I decided I’d better try to get some sleep.
About 2 a.m. things got exciting again. First, his diaper leaked. Right now, Patrick’s ostomy doesn’t have a bag on it (that’s a story in and of itself) and so I had to get up to change it because the combination of creams and powders required to protect the skin against what is essentially stomach acid is pretty complex and not your standard nurse’s experience.
While he was awake, they took his blood pressure and it was frighteningly low. They checked it about 20 times over the next stretch of time and even though he was awake and uncomfortable, which should raise blood pressure, his was low.
So they finally got his PICC line to draw back and drew some emergency labs to look for dangerous things like low blood sugar, drew blood cultures, and called the ICU to come look at him.
A doctor from the PICU came and looked at him and checked his blood pressure and said that he needed to go downstairs so they could give him medicines to bring his blood pressure back up.
So, at 3 a.m. we packed up and transferred to the PICU. It was odd to be there in my PJ’s giving his medical history. Finally at around 5 things were pretty stable and they recommended that I go get some sleep. So I went and crashed on one of the beds in the parent waiting room.
The next day they explained that sometimes infections cause your blood pressure to drop. Patrick responded very well to the medicines they’d given him, though, and was pretty stable. However, everytime he went to sleep, it would drop again.
Finally after being in the hospital for a full day, the antibiotics started to work. He started to act like he felt better, and his blood pressures came back up.
Thursday afternoon he was doing well enough that they moved him back from the PICU to the Infant Unit. Which is where I’m writing from tonight.
Patrick obviously feels MUCH better! He’s been back to trying to sit and stand and he’s getting stronger and more coordinated all the time.
The tentative plan right now is for us to go home Saturday. As always, when we leave the hospital, all of the nursing duties fall back on Brian and myself, with help from friends and family where possible. He’ll be on two antibiotics and an antifungal because of a diaper rash developing that is most likely yeast. (Antibiotics create the perfect environment for it to grow). With meds every 6 hours at least, sleep will become a very rare commodity again. Of course, as I’m posting this in the middle of the night, you’ll see that it already is.
We’re grateful that this bug seems to be one of the less scary ones. It’s called enterococcus, which lives inside the gut. It most likely either translocated (leaked) into the bloodstream from his gut or got in by accidental contamination of his IV tubing. Any way it goes, it required just 2 antibiotics to treat and Patrick’s central line so far can stay in. In those regards, we consider ourselves very lucky.
Of course we’ll do all we can to keep you updated on what happens from here. Thank you again for all of you do for us.
I need to stop promising to write about transplant. Whenever I do, Patrick gets sick and we end up back at the hospital.
Thursday in the middle of the night Patrick woke up crying the inconsolable cry he only uses when something is wrong. As usual, we immediately started looking for signs of a line infection. However, his temperature wasn’t even 100 degrees (100.4 is the least his doctors consider a fever) so we fed him a bit and I sat up with him and eventually he went to sleep.
When he woke up in the morning, something was definitely still wrong, but he still didn’t really have a temperature… just didn’t want me to put him down. As we always do when he’s sick, I held him and took regular temperatures. Around 10:30 a.m. his temperature hit the magic 100.4 and I started making calls to get blood cultures drawn. Usually we have some time if we catch it that quick. However, as I started to try to make plans, his fever kept rising. At 101 I started packing for the hospital, at 102 I put some hustle into it and by the time we made it out the door his temp was 103.
Being our 3rd fever in a month, I wasn’t too happy about the return trip to Primary Children’s.
When we arrived they checked his vital signs and then they did something they’ve never done before… instead of finishing the standard check-in process, the triage nurse disappeared for a minute and then came back and took us straight to a room. And not the typical room, either… They took us into one of the “resuscitation”, a.k.a. trauma, rooms. Patrick’s temp was over 104 and his pulse near 200. He had a serious infection and was in shock.
They quickly worked to cool him down with cold packs and fever reducers and eventually he was looking and feeling better.
Labwork revealed that Patrick had a yeast infection in his central line. Since yeast gets into the plastic of the line, it had to be removed. It has to stay out we are sure the infection is out of his blood. In the meantime, he has a peripheral (in the hand or foot usually) IV. You can’t give full TPN through this type of IV so he’s getting a sugar/saline solution instead.
So now we are in the hospital waiting out the infection so that Patrick can get to feeling better. He doesn’t get as much sugar as he’s used to so he’s lacking energy. The IV antifungal medicine upsets his stomach we think. He’s getting rather stir crazy. The two things that bother him the most, though, are 1) the blood draws they wake him for at 6 a.m. every day and 2) the splints on his foot and hand to keep him from damaging his IV.
He’s just not himself these days. Keeping him calm is a 24/7 job for me. I’m basically living at the hospital while Howie works, manages the house, and does his best to take care of me. But we can’t imagine doing it another way… Patrick is fighting hard to get healthy and needs support in the fight.
I have to share one example, though, of Patrick’s indominable spirit. This morning we added the IV to his hand and so he woke up to having a splint put on that immobilizes his left hand. For the first part of the day he’d look at his hand and just whimper… he’d try his best to hold it still. Finally later in the day the nurse helped me get some toys that work with the touch of a button so he could use his splinted hand to play with them. After some work with that he started to get a little more adventurous.
He got a wrapper in his free hand and was playing with it and, after some work, he managed to hold the wrapper with the fingers on his splinted hand. He worked on that for a good 15 minutes, then he reached over and grabbed my hand with his free one. Using his new skill, he put my finger where he could hold it with the fingers of his splinted hand.
Patrick is an amazing kid. This is one of the hardest trials we’ve seen him go through so far… However, tonight’s adventures show me that he is determined to push the limits that his imperfect little body give him.
We hope that he’ll be able to stay healthy for a couple more days, have a new line surgically placed midweek, and then be able to come home for the final weeks of his recovery from this infection. If any little spirit is strong enough, Patrick’s certainly is.
 Chicken and I had the opportunity to go to church at the hospital today (for those who haven’t heard, Patrick is in the hospital, but those details will come later). While we were sitting there a lot of emotions regarding fathers day came to mind. I thought that I would try to write some of those down.
Chicken and I had the opportunity to go to church at the hospital today (for those who haven’t heard, Patrick is in the hospital, but those details will come later). While we were sitting there a lot of emotions regarding fathers day came to mind. I thought that I would try to write some of those down.

Tuesday morning found us back at Seattle Children’s again bright and early. Our day started in ultrasound. They wanted images of his digestive system and the central-line eligible veins in his neck. With so much to image, we had 3 hours scheduled with ultrasound.
Keeping a 6 month old still for 3 hours while goop is being rubbed around on his abdomen and neck is quite the feat. We went through every toy that I’d brought along… rattles, books, rings. In the end, the only way to keep his head still for images of his neck was to let him watch my cell phone’s media player. It was interesting to watch them map the flow of blood through his veins and to see his broviac line. Patrick was a big fan of the black and white images on the screen.
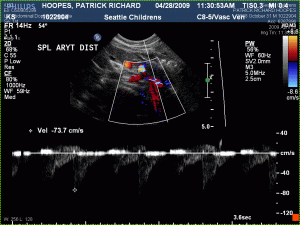
In the end, the ultrasound took 3 and a half hours, not 3, and we had to run to make our next appointment with the department social worker.
Because the transplant process can turn your life completely upside down, part of the workup is a meeting with the social worker. She asked a lot of questions about us to make sure that we were up for the task. We talked about our coping mechanisms, our family, friends and other support systems. She told us about programs in place that could help us like the Ronald McDonald house (as a place to stay during Patrick’s recovery), Angel Flight (for transportation to and from many doctor’s appointments in Seattle, and the Children’s Organ Transplant Association(a.k.a. COTA, a charitable organization that will create an account to save and fundraise for transplant in). The social worker will be our go-to person for a lot of the logistics of planning and paying for the transplant, which will be invaluable, as this is not easy or inexpensive by any means.
Because we were running late, the appointment with the social worker was divided in two to give us the chance to meet with the surgeon, Dr. Reyes. Dr. Reyes is an expert in intestinal transplant. He’s originally from Brazil but you’d never guess it from talking to him. He explained to us a little bit about how the transplant works. He also explained the difference between an isolated intestine transplant (intestines only) and a liver-intestine transplant. The first would be done if Patrick’s liver were still in good condition. The chances of rejections are a bit higher, but if the bowel were to be rejected, they could remove it and wait for another donor. The latter would be done if his liver is in bad condition. The liver, pancreas, and intestine would all be transplanted at once, still connected to each other. The liver helps to protect the other organs from rejection – but if it is rejected, then the chances of finding another donor before the situation becomes fatal are pretty slim.
We were surprised when he asked us if Patrick’s small and large intestines had been connected. We had been previously told this wasn’t possible because the small intestine was oversized and the large intestine was pencil-thin from lack of use. But Dr. Reyes thinks it would be very beneficial to connect these. Patrick has a good portion of colon left that could help absorb water so that fluid loss would be less of a concern for Patrick and we could perhaps feed him more. This wouldn’t eliminate the need for transplant, but would reduce some problems in the time we’re waiting.
After wrapping up with the social worker, we ran over to neurodevelopmental. There a developmental specialist met with us. She took a quick history while we fed and changed Patrick, then she did her evaluation. This was probably his favorite appointment. Basically, she played with him to see what he knew how to do. The funniest was when she was testing his verbal repetition. She’d say “Aaaa…. Now your turn” and he’d respond by blowing raspberries back, since he’d just learned to repeat that sound and was quite proud of his new skill. In the end, her analysis was that he lacks some muscle tone, but that he is developmentally right on target for his “adjusted age”… meaning you subtract 3 weeks from his age because he was born 3 weeks early and he’s just where a 5 month old would be.
Our last appointment of the day was with Dr. Horslen the gastroenterologist. Dr. Horslen is one of the best known gastrointerologist in the world of short gut syndrome. He is from England and just transferred to Seattle from the very established program in Omaha, NE. He is oozing with British-ness. Patrick was finally napping by the time we got to that appointment so he slept while we repeated Patrick’s medical history again. Then Dr. Horslen examined him and he woke up and gave him a big grin. Dr. Horslen labeled him a charmer from the start.
Dr. Horslen told us that he and Dr. Jackson (our GI in Utah) have known each other since Dr. Horslen first arrived in the U.S. and said he respects him very much. He is very willing for the 2 of them to work together as a team. He did go on and tell us what changes he’d make if he were treating Patrick in Washington. 1) He said he’d reconnect Patrick’s intestines. (Which made us happy to hear… we’re excited about this possibility.) He explained that not only would Patrick have less water loss this way, but that the stoma can start to bleed uncontrollably as the liver fails… something that there’s no real reason to put Patrick or us though. 2) He suggested that we follow some of the suggested changes in diet and TPN. 3) He said he’d replace Patrick’s lipids with Omegaven (a topic I’ll have to cover in another post). They’re doing a study at his hospital and he’s allowed to distribute it in the state of Washington. 4) He’d do a contrast study of Patrick’s intestines… (Also to be explained later)… basically, take some images to see what’s there.
Then he threw in a 4 that we’d been expecting since the social worker ran into us at dinner and accidentally let it slip… He needed to see Patrick’s bloodwork right away to know what else needed to be done… And since Patrick was VERY anemic… He’d admit him to the hospital that same night so he could have a transfusion after the blood was drawn. They had a room ready for us to be admitted that night.
Now, in the interest of keeping this blog readable, for it’s length… and just for the fun of the suspense… I’m going to leave you in that cliffhanger until I find time to write again.

So the first big question about getting Patrick to Seattle was transportation. With current airport security, how do you get a kid who is connected to running IV fluids through security? And how do you go about transporting a week’s supply of TPN? It has to be kept at a certain temperature and, well, there is just a lot of it. Hauling a cooler and coordinating tubing through the airport just didn’t sound like much fun to us, but neither did dealing with any lost luggage.
So I did tons of research: called the TSA, read every page in the Delta website about baggage, and read websites written by other TPN patients. Finally, I asked the pharmacy if they could ship the TPN ahead of us. Turns out, that’s a free service that they provide. And our wonderful friends Lindy & Kelly helped us find a place in Seattle to ship to and then picked up the shipment and kept it in their fridge until we could get there.
So we were able to travel with just 2 day’s worth of medical supplies in our carryon… which was still enough to fill an entire carry-on sized suitcase, but probably saved us TONS of grief. Patrick’s luggage was by far the biggest and we were probably quite the sight making our way around with Howie hauling 3 rolling suitcases behind him and his carry-on and me with a stroller, a duffel bag, and a diaper bag.
We were surprised by how smoothly things went at security. In Salt Lake a TSA worker came up to us when she saw us getting our stuff ready to go through X-ray. I explained to her Patrick’s IV’s and showed her my suitcase full of medical equipment, including IV solutions and syringes full of saline and heparin. She took over right away. Patrick and I went through the metal detector and (of course) set it off because of his pumps. Then they took us to the little security station and ran their little tests on his medicines. When they were all done, they patted Patrick down and then did a wand/hand search of me. Then they thanked us for keeping things organized and making them easy and sent us on our way.
We were allowed to board the plane first because we were travelling with an infant, which was different but nice, especially since we needed to get his stuff settled so we could get to anything he needed during the flight.
We booked him a seat, not to sit in, but to give us some extra space. His backpack rode there buckled in and Patrick started the flight in his daddy’s arms. He played and he slept and he flashed his bright eyes and smile at the flight attendants and the passengers around us. He was by far the best behaved child on the flight! Whimpered only when he was hungry.
Finally we landed and took our crazy little caravan to the rental car company and checked in at our hotel. We took a much needed nap before heading over to visit Kelly and pick up the TPN shipment.
The day of travel was much smoother than I could have ever expected! Which turns out to be a good thing, as we had a very long week ahead of us
We’re going to have a little series of posts here about Patrick’s transplant pre-evaluation at Seattle Children’s Hospital. I decided to break this up into a series not to extend the suspense for you, but to increase the odds that I would be able to finish a post in a single sitting.
So, we’ll start with an introduction. As you know, Patrick has extreme short gut syndrome. Without intestines, he is completely dependent on TPN for nutrition. And the lipids in the TPN are notorious for damaging the liver. If he had more intestine, there would be the option of adapting Patrick’s intestine, but with so little, he needs to have a transplant before his liver fails if he is going to survive.
Our GI in Utah recommended that we go to Seattle Children’s Hospital where they have a relatively new intestinal transplant program being started by some of the most experienced doctors in this field in the country. So, after some prayer and some research we requested a referral and last week we flew out for an evaluation.
There are several purposes for a pre-evaluation for transplant:
1) It gives us a chance to meet the team and see the facility and decide if we want to pursue treatment there.
2) The doctors can see the patient and have tests done to give them first hand knowledge of the case so they can recommend a plan of action, including deciding if transplant is the only option for the patient.
3) They do lots of tests that check to make sure Patrick is healthy enough for a major surgery, to detect any unknown health problems, and to gather the information needed to match him with a donor.
4) They look at our family’s ability to maintain Patrick’s care financially, emotionally, and physically both before, during, and after transplant.
Once the workup is complete, Patrick’s case is presented to a review board and a decision is made as to whether or not he is a good transplant candidate. When the decision is made, they’ll notify us.
So that’s the purpose of the pre-evaluation. The next few posts will describe our experience and what we learned.
We’ve been a very busy little family lately. Patrick is 5 months old now. And in the time since I last posted, we’ve had a lot of firsts. So, here are some highlights.
 First giggles
First giggles
Patrick learned to laugh a while ago, but we didn’t get out and out chuckles until we discovered that the kid who used to scream his head off whenever he got undressed is ticklish and loves to have his clothes off. Dressing and especially weighing are now favorite games… but it’s best when daddy just picks him up without clothes on and tickles his back.
Today we learned that you can also get belly laughs if you squish his cheeks.
 First fever
First fever
Well, it all started with a cold, that turned into croup. After a week and a half trying to fight it off, Patrick got his first fever. Fortunately, it didn’t go much higher than 100.4 (38 degrees Celsius) and so we were able to have blood cultures drawn at home and his fever was gone in a day. No infection, thankfully. Just a day at home with Mom holding Patrick and taking his temperature every half an hour to make sure it hadn’t hit the danger mark yet.
 First necktie
First necktie
My brother Steven got married at the end of March. Although we were crazy busy working on his wedding cake and pictures, I just couldn’t help taking the opportunity to make Patrick and Brian matching neckties. We bought a tie with a matching handkerchief. Patrick thought his tie was a great toy to hold and chew on.
Oh, and a disclaimer on this picture. Patrick hates bright lights of any kind and we had studio lights on. Someday we’ll get a family picture with him not crying.
First rollover
I set Patrick down and turned my back on him for just a minute. When I turned back, he was on his tummy looking up at me as if to say “Whoa, Mom! What do I do now?” So far no signs of him having any idea how he did this or how to do it again. But we’re having much more play time on the floor to encourage him.
First haircut
After weeks of trying, we finally got time to take Patrick to my Grandpa’s house for his first haircut. In my defense (for those of you who thought I should never cut it), his hair was in his eyes and under his chin. Patrick was ok with the whole haircut idea till we hit the ticklish spot behind his ears. Finally, though, he fell asleep and we were able to finish. It’s a nice short cut.. but we hope that means it can grow for a while again before it needs another cut.
First ER visit
Last Saturday night, I noticed some bleeding under the dressing for Patrick’s central line. The line had shifted and, on closer inspection, we found that it had been pulled. It didn’t pull out, but was far enough to worry us. So – we got to make our first trip to the ER.
We were probably quite the sight there because, unlike the other families, we weren’t panicked. Central line issues are just part of life with Patrick. We’ve been planning and practicing for this trip for a while.
We arrived at 10:30 p.m. and had a bit of a wait in the waiting room because we were definitely not the most urgent case there. They took some x-rays to see the position of the line and about 1 a.m. the surgeon who placed Patrick’s line came into the room. He had been called in for an emergency appendectomy, and stopped in to see Patrick while he was there. He looked at it and said that the line was in a good position and he didn’t think it needed to be replaced on an emergency basis. Instead, we were to put antibacterial ointment on it twice a day to prevent infection, which meant lots of dressing changes, and then get a second opinion on Monday.
We were amazed, but happy, and after teaching an E.R. nurse proper technique for dressing change (yes, us teaching her), we were sent home. We got home at 3:30 a.m., connected Patrick’s feeding tube, and slept in till 11:30 a.m.
 First outpatient surgery
First outpatient surgery
So that brings us to Monday. About a month and a half ago we started the battle of the granulation tissue. Patrick had a patch of it next to his stoma that just kept growing back, no matter what we did. We learned to use silver nitrate to treat it, but it just kept coming back. So – we decided that maybe it was doing no harm and we’d leave it as it was.
No sooner had we made that decision than I discovered that his g-tube was surrounded by granulation tissue. A visit with the nurse practitioner in the GI clinic taught me better technique for nitrate treatments and after 10 miserable days of treatments, his G-tube site was clear of it. However, the spot by his stoma was starting to make it hard to keep a bag on and his skin was getting sorer by the day. I tried my newly practiced skills, but the tissue just kept coming back
So, we called and scheduled an appointment to have it electrocauterized. This is a minor procedure, but it’s painful and so they put babies to under so they don’t have to suffer through it. The surgeon we saw in the E.R. told us to as for follow-up at our appointment on Monday. It was still looking sore and red and swollen and the surgeon didn’t like the look of it, so he decided it was best to change the central line.
 This means that they took it out of one vein and put it into another one, coming out in a different place on his chest. Again, this is something we’d been warned about, so it wasn’t a complete shock. However, we were a bit nervous and, after an already long weekend, quite tired.
This means that they took it out of one vein and put it into another one, coming out in a different place on his chest. Again, this is something we’d been warned about, so it wasn’t a complete shock. However, we were a bit nervous and, after an already long weekend, quite tired.
The surgery went well. Patrick woke up and was able to come off the ventilator in no time at all. He was, as always, a favorite with the nurses in post-op. Brian got to reconnect his TPN in post-op, which was kind of funny to do. Our nurse was fascinated with the different equipment. We got some curious looks as Brian drew up vitamins with syringes and injected them into the IV bags.
 It’s a curious thing to be the old pro parents in the hospital. I often refer to myself as a “hospital mom”. We know the routine. We’re patient with the nurses, doctors, and other staff and, although we are concerned for Patrick, we are not scared or intimidated by our surroundings as we once used to be. It’s kind of odd to feel perfectly at home in a hospital… But makes all of this more bearable.
It’s a curious thing to be the old pro parents in the hospital. I often refer to myself as a “hospital mom”. We know the routine. We’re patient with the nurses, doctors, and other staff and, although we are concerned for Patrick, we are not scared or intimidated by our surroundings as we once used to be. It’s kind of odd to feel perfectly at home in a hospital… But makes all of this more bearable.
Patrick was sore and tired for a day and still whimpers if we move his not-quite-healed shoulder the wrong way… But overall he’s back to himself. As for Howie and myself, well, we’re slowly but surely catching up on our sleep and getting back to a normal routine. And preparing for the adventures ahead.
First steps to transplant
And that brings us to the last of the firsts for this entry. We have made the first steps towards transplant evaluation for Patrick. We have appointments for April 27th and 28th at Seattle Children’s Hospital to meet with the surgeon, gastrointerologist and just about anyone else who might have anything at all to do with Patrick’s transplant. Theevalution process is big, long, and very detailed. They want to make sure that Patrick needs and will benefit from a transplant, that he’s healthy enough to have one, and that his home life lends itself to as successful of a recovery as possible. This trip is the first step in that process, and we are excited to go and learn and start building relationships there.
Patrick still has a long way to grow. He’s almost halfway to the 10 kilo weight goal. (He weighs 10 lbs 11 oz.), and so we know this visit won’t end with him on a list. But it’s a start and a step in the right direction.
And so, those are the firsts we have to report for the time being. We’re looking forward to continuing to see him learn and grow. He is so good at using his hands now! And has just started to discover that he has feet. His spirit grows by leaps and bounds every day. Most of all, he amazes us with his incredible patience and optimism.