Or perhaps I should title this post “A date with the devil.” We are being forced to get to know the devil we don’t know.
Believe it or not, we finished a course of antibiotics and we went on vacation. Brian went on a business trip to the Ukraine. Patrick and I went to visit our good friends, the Laylands, in Seattle.
But writing about those things will end up waiting for another day. Because I’m writing tonight from a hospital room. Again. And there are things on my mind that, for me, have been the subject of nightmares for many months now.
Patrick has lost his central line. Not entirely yet. But it will have to be replaced.
It all started Saturday night right after I put Patrick to bed after our first day home from Washington and went to clean up before Brian returned from Ukraine. Patrick had been in bed about half an hour when I heard a plaintive “Mommy”, and then that unmistakable, heart stopping sound of him throwing up in bed.
I ran up the stairs but was too late. The poor little guy threw up half a liter of nasty green stuff. He must have felt awful all day. It took an hour to settle him enough to sleep.
Saturday morning, a homecare nurse had come to draw some labwork and follow up blood cultures. All seemed well at that point.. But i was very glad for those cultures when Sunday morning, Patrick was having low grade fevers. We went to church just to be able to take the Sacrament and see how long we could make it. We had a backup plan for our assignments at church.
And it wasn’t long before it was obvious Patrick didn’t feel well enough to sit quietly. So I took him to the foyer to let him move and I got on the phone with his doctor to see if we could come get more bloodwork done. And I pulled out a thermometer, and there was the number we had waited all morning for. 100.4 degrees farenheit. And official fever.
So, we made a bit of a scene leaving church, packed bags, and came to the hospital.
It took several hours to restart Patrick’s antibiotics. 8 for the one I thought he needed most, which just about made me crazy waiting for as he got feeling sicker and sicker. But as soon as they were given (along with a Priesthood blessing), Patrick started to feel a little better. We even slept through that first night.
All seemed to be going smoothly by the end of the 2nd day. I was a rockstar advocate mommy and got Patrick therapy, a picture schedule, integrative medicine & aromatherapy, and even talked to the palliative care team about signing him up for their services. I even managed to get his GI, surgeon, and a radiologist to have a care conference to discuss replacing Patrick’s positional line. They came back in favor of a change and suggested a plan of action to decide if and how to proceed.
And then, at 4 p.m., we came back to the room to draw cultures and start his antibiotics and his line wouldn’t draw. Or flush.
We ordered TPA and we worked it, and we worked it… and, well, after 4 hours of effort, he was exhausted, I was heartsick, and the line was still not working. And the plan from the care conference was upgraded from a hypothetical, optional plan to a necessity.
I did not sleep as well last night. (And not just because the nurse was slow about keeping the pumps from alarming and banged the door.)
Today we put the plan into action. Patrick went to radiology for a sedated ultrasound of the veins in his upper body. The order was for light sedation.
We learned today that Patrick is very capable of fighting light sedation. Made him silly and sleepy, but he was still perfectly able to fight the test. Moderate sedation didn’t fix things either. In fact, with sedation all of his inhibition control was gone and none of my usual distraction tricks were even an option. The ultrasound was wiggly, to say the least.. but the technician was patient and kept trying to get the information the doctors wanted.
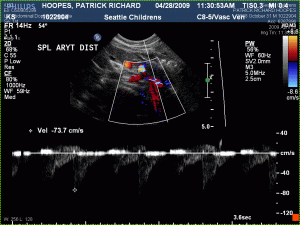
Listening to her review her images with the radiologist, though, made my heartsick. As usual, Patrick’s right side vessels are fairly scarred. (Though perhaps a little better looking than the last I’d known.) But, they worked enough to give a better answer about the left side than before. Instead of just saying “Inconclusive”, what they said was that the left subclavian vein (the one in his shoulder) has lots of little collateral vessels around it too and shows evidence of being swollen at least, if not scarred, and also probably has a clot in it.
I asked the radiologist if that would explain the tricky behavior of this line for the past year and he said absolutely, that the vessel may have been pressing on the line. He also said that changing out the line over a wire was a risky move, given the clot in the line. But that I’d need to discuss that plan with our surgeons.
Other vessels were open, but most of them looked to have some kind of narrowing.
The rest of the afternoon was a little crazy. I got permission to change out Patrick’s button while he was still sedated and that went quickly and smoothly and he doesn’t seem to understand it even happened. That’s what we hoped for.
And that meant that Brian came up for the ultrasound and stayed the afternoon.
But it was a rough afternoon. Patrick didn’t sleep under sedation and he didn’t sleep after, either. He fought REALLY hard all afternoon to stay awake. We could tell when it started to wear off because he finally stopped fighting.
But because of low heart rates, he still had to stay in bed till 5:30. We got out for a short walk, but when we came back for TPN at 6, and I asked the nurse if all was done so we could leave, she told me no. She didn’t want to use the automatic settings to taper Patrick’s TPN levels up (to protect his blood sugar levels)… and so, we couldn’t leave the room.
The idea of making Patrick stay any longer in the room with the same old toys and bed and short IV tubing kind of broke my heart. So I had a very short little cry about it. Then I went and helped myself to several fitted sheets and used the extra safety pins around the room to build us a fort.
That tided us over for the rest of the evening.
Tomorrow will not be an easier day. As of tonight, they plan to take Patrick to surgery tomorrow. The surgeon will probably attempt first to put a line back into the same vein. That means that he’ll put a wire into the catheter, remove the old line leaving the wire, and then use the wire to guide a new line in.
That is the best case scenario.
The worst case scenario is that that won’t work. In that case, they want to repeat a venogram.. which is a contrast study of the Patrick’s veins. And they will use that to pick a new vein to put a line into.
It is entirely possible that the surgeon will come in in the morning and decide that he wants to have that done before Patrick goes to the OR. And then we’ll just do that tomorrow and the surgery the next day.
And the worst of worse case scenario is that the wire over doesn’t work, none of the other vessels are still wide enough to get a central line into, and then we’ll start discussing desperate measure that I don’t really want to get into in a blog post unless they happen.
Needless to say, this is scary. I am still terrified of the idea of Patrick no longer having veins to give nutrition through. I do not want to imagine that happening.
We are not to that point yet. There are veins in other places in the body that can be used. But there is still a lot of pressure to make one of these sites work because in order to have a transplant, Patrick has a have a central line in his upper body.
I’m scared and I’m sad.. and I’m really, really lonely for some reason this stay. But I’m calm. We have been praying and fasting about this line for a while now. I can’t help but think that this is an answer to those prayers.
So, if you’re the praying type, please join us in praying for the surgeon and his team and the radiologists tomorrow. We’d love to save this access site. We’d love to get another year and a half or more out of another. And I have this faint little hope that maybe the next line won’t scare me every time someone else flushes it, (and sometimes when I do, too.)